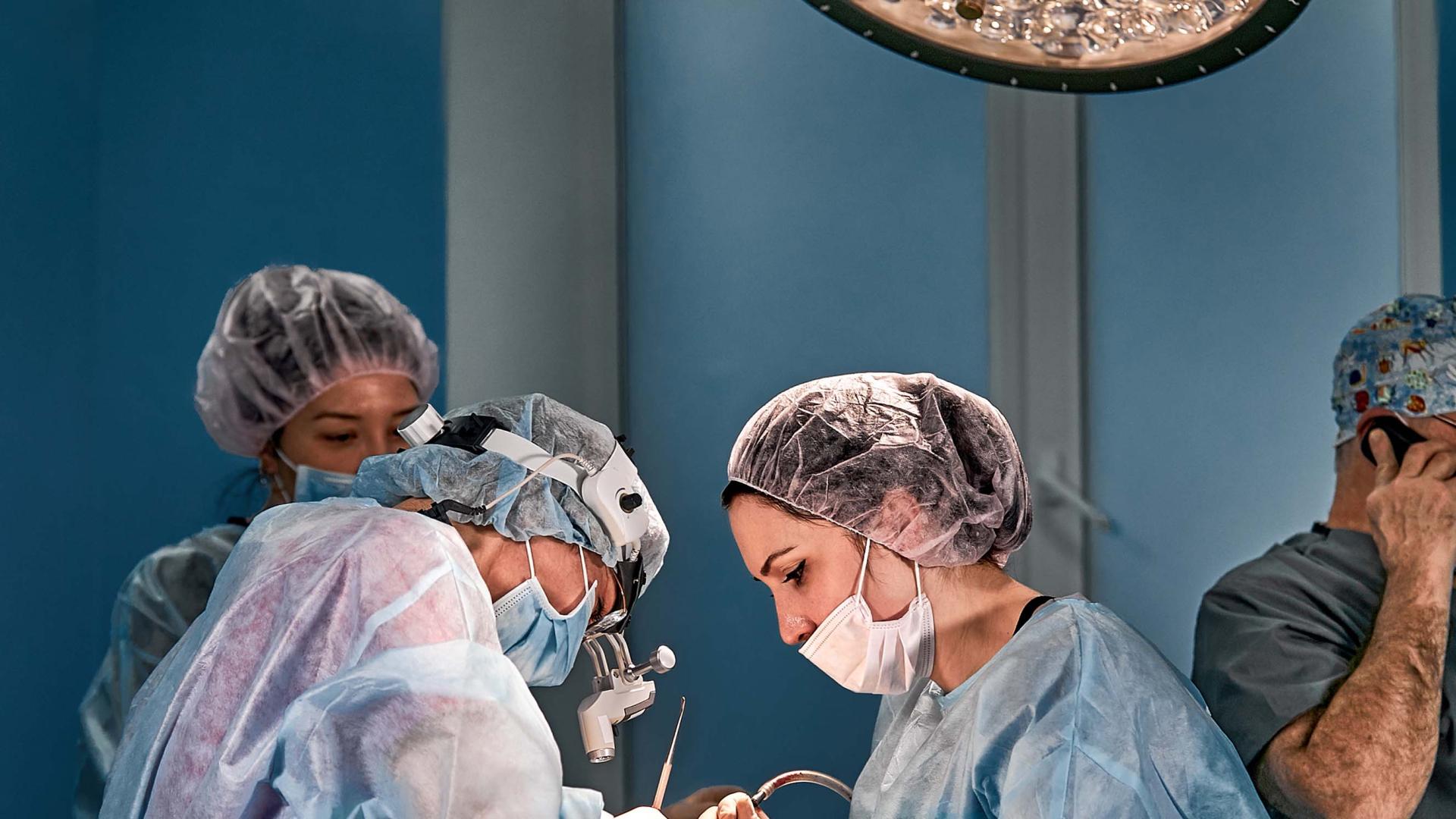
Survey evidence published recently showed staggering levels of sexual harassment (and worse) in surgery.1 Evidence from the Institute for Fiscal Studies shows that surgery is also an environment where combining motherhood with a medical career is particularly challenging. Women in male dominated medical specialties, including surgery, have fewer children and take shorter periods of maternity leave than women in other specialties.2 Mothers in surgery work more hours after returning from leave than those in other specialties.3
We are unable to unpick whether these differences reflect choices imposed on women by the structure of surgical training or the working culture. But they do contribute to the overall picture of an environment unwelcoming to many women and not sufficiently supportive of their needs.
Given that female surgeons take less parental leave and are more likely to work full time, one might expect their career progression to be harmed less by parenthood than mothers in other specialties. Our analysis suggests the opposite is true. Across all specialties, rates of progression from core to higher specialty training are lower for women returning from maternity leave than for childless men.4 But the relative falls in progression rates for mothers in surgery are double those of mothers in non-surgical specialties.
Adjusting for lower levels of accumulated experience - through parental leave and part time working - explains the relative slowdown in progression for mothers in non-surgical specialties. In surgery, it explains very little, as gaps in accumulated experience between parents and non-parents are much smaller.
An environment that enables women to have successful careers in surgery is both right and essential if the NHS is to make the best use of available talents. There might be some necessary features of surgery that make balancing it with parenthood harder. But this seems far from the only factor explaining why rates of women specialising and progressing in surgery remain low.