The long-term care needs of the older population are of considerable societal and policy interest. For many years, there has been debate over unmet need for social care and over problems with how care services are funded and how the cost is shared between private individuals and the state. These issues were always expected to increase in importance as the population aged and demand for services increased. Concern has increased in recent years, in the light of cuts to public spending on social care that have formed part of the government’s budget cuts in the wake of the financial crisis. Greater understanding both of the underlying trends in care receipt due to demographic change and of how public spending cuts are likely to impact on individuals’ care receipt and subsequent health and well-being, is therefore now of considerable importance.
Until recently, consideration of a holistic picture of social care receipt was inhibited by data availability – specifically, a lack of reliable data on people who fund their own care, particularly in a household setting. However, the inclusion of questions on the need for, and receipt of, social care in large-scale household surveys (such as the Health Survey for England and the English Longitudinal Study of Ageing) has helped to address this. Such data have now been used by a number of researchers to examine care receipt among the older population. This existing research has found that care receipt is strongly associated with need (typically measured by difficulties with daily living) and that different types of care are more associated with different dimensions of need (for example, informal and publicly-funded support are more often received by those with difficulties with basic tasks such as bathing and getting dressed, while privately-funded support is more often received by those with difficulties with activities such as shopping and housework). Other demographic and socio-economic characteristics are also important – wealthier individuals are more likely to receive privately-funded care and less likely to receive state-funded care, while those without partners or children are less likely to receive informal care.
These existing studies typically examine the receipt of care, and the factors associated with this assistance, at a given point in time. However, care is a dynamic process, with the need for and receipt of care changing as individual circumstances develop over time. Understanding the factors associated with changes in the receipt of assistance over time is therefore important for policy and, until now, they have been underexplored.
In this report, we use data from the English Longitudinal Study of Ageing to examine the prevalence and dynamics of social care received in private households. We use the latest available data to update existing evidence on the prevalence of receiving help with certain activities among the older population. Specifically, we describe, for a given point in time, who receives help, what type of help is received, how many hours of help are received from different sources, and the role of local authorities and private finance. We also exploit the longitudinal nature of the data to provide the first evidence on the dynamics of care receipt in England: how the proportion of individuals receiving domestic care changes when we consider a period of time rather than a snapshot, and what characteristics and factors are associated with starting and ending care receipt. Finally, we consider how the receipt of care differs across different date-of-birth cohorts, the possible drivers of this variation and its potential implications in the context of an ageing population.
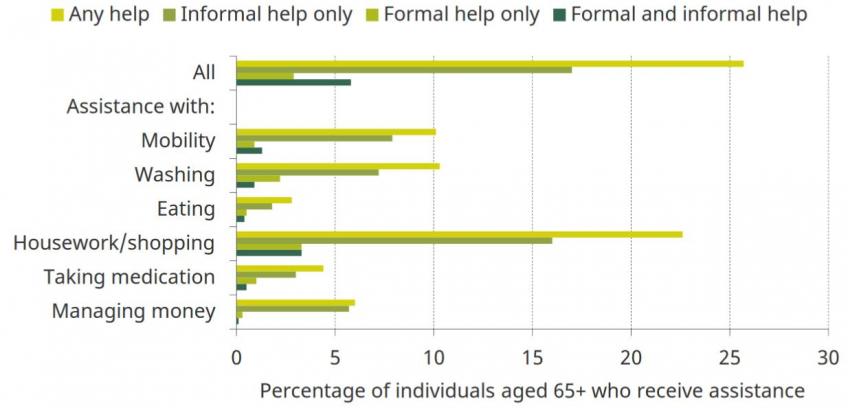
Figure. Receipt of assistance in the last month, by activity category
This report was funded by the Health Foundation as part of a broader programme on the allocative efficiency of health and social care spending. The authors also gratefully acknowledge co-funding from the Economic and Social Research Council (ESRC) through the Centre for the Microeconomic Analysis of Public Policy (CPP) at IFS (grant number ES/M010147/1) and the 'Policies for longer working lives: understanding interactions with health and care responsibilities' project (grant number ES/P001688/1) that is part of the Joint Programme Initiative “More Years, Better Lives”.










